Pakistan's Recurring HIV Crisis Exposes Systemic Healthcare Failures
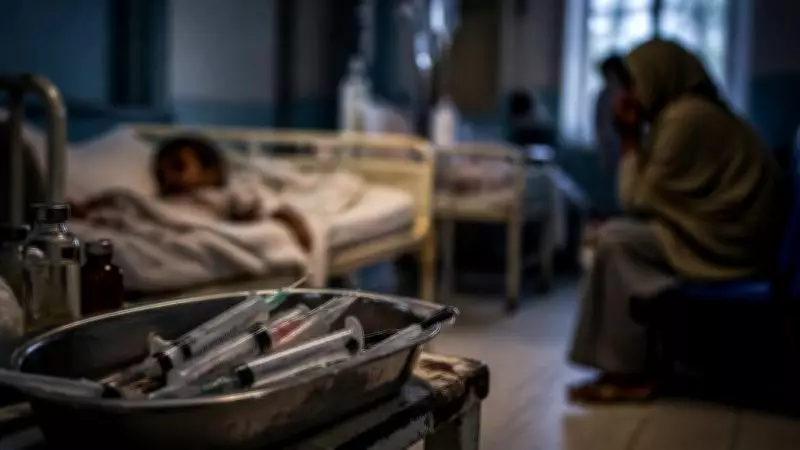
Every few years, Pakistan confronts a devastating health crisis that it has previously encountered, and this week, the alarm is sounding once more from Punjab. A recent BBC investigation has reported that at least 331 children in Taunsa tested HIV-positive between November 2024 and October 2025. Shockingly, staff at a government hospital were filmed reusing syringes and violating basic infection-control protocols, practices that have dire consequences for public health.
Urban Spread and Rising Cases Across Major Cities
Meanwhile, Karachi is experiencing a sharp increase in paediatric HIV cases, with Dawn reporting 159 patients admitted across three city hospitals this year. Most of these infections are linked to unsafe healthcare practices, underscoring a widespread issue. Even more troubling is that the epidemic is no longer confined to peripheral areas. Islamabad recorded 618 new HIV cases between January 2025 and March 2026, with adult men constituting the majority of infections. This development is significant because when HIV rises in the capital, a posh urban center, it transforms from a local failure into a federal warning about urban transmission, surveillance gaps, and a system that is failing in plain sight.
Historical Context and Preventable Patterns
The first point to emphasize clearly is that this story should not be reduced to sexual panic, gossip, or blaming marginalized groups. The World Health Organization (WHO) states that HIV in the general population can spread through unsafe injections, unscreened blood, and poor infection control. Specifically, WHO notes that the 2019 outbreak in Ratodero was attributed to reused syringes for therapeutic injections, making the needle a central issue rather than a side note.
Pakistan has traveled this painful road before. Reuters reported in 2019 that nearly 700 HIV cases emerged in Ratodero since April of that year, most involving children. WHO's later review found 876 people tested positive in Larkana district between late April and late June 2019, with 719 being children. Crossing borders, a similar pattern is evident; Reuters reported in 2018 that at least 33 people in Bangarmau, India, tested positive after an unqualified practitioner used an infected syringe. This repetition highlights institutional memory failing in real time, where public health should learn from past outbreaks to prevent future ones.
Cultural and Systemic Factors Driving the Crisis
The deeper problem extends beyond mere malpractice to a culture that normalizes such practices. Studies in Pakistan reveal that injections are overused, with many patients believing they work faster than tablets and are less risky than oral medicine. WHO's review of syringe reuse in Pakistan indicates that patients often expect injections for minor ailments, and providers comply with this demand. This reflects a blend of ignorance, habit, and medical superstition, where injections are perceived as symbols of expertise and decisive treatment.
In Pakistan's medical culture, the doctor's authority is rarely questioned, leading patients to defer to expertise rather than demand safety. Additionally, financial incentives play a role, often involving small savings from reusing syringes, hidden from patients. WHO's 2020 review warns that laws or auto-disable syringes alone will not solve the issue without patient awareness and systemic changes. This corruption is not always dramatic but can involve minor negligence with catastrophic effects, such as infecting a child and altering their life forever.
The Impact of Stigma and the Path Forward
Stigma adds a second, deeper wound to the crisis. HIV stigma in Pakistan is real and corrosive, particularly regarding disclosure to family and social contacts. It pushes families into silence and shifts public debate toward moral theater instead of practical reform. Instead of focusing on why hospital wards reuse syringes on children, discussions often center on shame, which is an ineffective public-health policy.
If there is any lesson from this recurring tragedy, it is that Pakistan cannot continue treating HIV outbreaks as isolated scandals. They are symptoms of a larger systemic failure where the health system is too comfortable with injection reuse, too tolerant of quacks, too weak on inspections, and too quick to moralize crises. The solution lies not in another round of outrage but in boring, relentless discipline: ensuring single-use equipment is actually single-use, extending inspections to private clinics, implementing blood screening, providing infection-control training, and launching public messaging that removes shame from HIV and focuses on unsafe practices.
Pakistan already knows the diagnosis for its recurring health crises. The true tragedy is the persistent delay in administering the necessary treatment to prevent future outbreaks.









